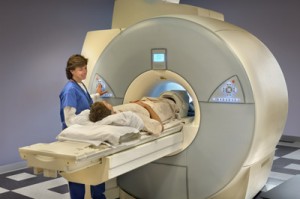
How Does An MRI Work
When doctors need the highest quality images possible they turn to MRI scanners, but how do they work?
Doctors often plan treatments based on imaging X-rays, ultrasound and CT scans provide useful pictures, but when the highest quality images are needed, they turn to MRI scanners.
While CT scanners use x-rays and therefore expose the patient to radiation, magnetic resonance imaging (MRI) uses powerful magnets and is virtually risk free.
MRI scans are obtained for many medical conditions, although since they are expensive and complicated to interpret, they certainly aren’t as easy as taking a chest x-ray. Examples for which they are used include planning surgery for rectal cancers, assessing bones for infection (osteomyelitis), looking at the bile ducts in detail for trapped gallstones, assessing ligamental damage in the knee joints and assessing the spinal cord for infections, tumours or trapped nerves.
Physicists and engineers use and manipulate the basic laws of physics to develop these incredible scanners for doctors to use. MRI scans provide such details because they work at a sub-molecular level; they work on the protons within hydrogen atoms. By changing the position of these protons using magnetic fields, extremely detailed pictures of the different types of pictures are obtained. Since these pictures rely on the tiny movements of these tiny particles, you need to lie very still during the scan.
![How Does an MRI Work How Does an MRI Work]() Slice by slice images
Slice by slice images
Specially wound coils, known as gradient coils, allow for the detailed depth imaging which creates the slice by slice pictures.
While the main superconducting magnet creates a very stable magnetic field, these gradient coils create variable magnetic fields during the scan.
These fields mean that the magnetic strength within the patient can be altered in specific areas. Since the protons realign at different rates in different tissue types, the relationship between the strength of the field and the frequency of the emitted photons is different for various tissues. Detecting these differences allows for very detailed images.
Powerful computers outside the main machine then reconstitute all of this data to produce slice by slice imaging. Depending on what’s being scanned, 3D reconstructions can then be created, such as for brain tumours.
Planning from the detail
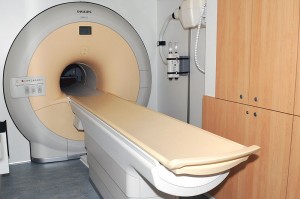 The detail provided by MRI scanners enables doctors of all specialties to plan their treatment. When footballers damage their knees, an MRI scan will tell if the ligaments are ruptured.
The detail provided by MRI scanners enables doctors of all specialties to plan their treatment. When footballers damage their knees, an MRI scan will tell if the ligaments are ruptured.
Knee surgeons can then reconstruct the damage, often via keyhole incisions (arthroscopically). MRI scans are used to characterize a variety of tumours, such as those of the rectum (the lowest part of the colon) and within the brain.
MRI gives enough detail to determine the size and stage of the tumour. This helps specialist surgeons plan whether the tumour is resectable, and also how to perform the operation.
The MRI’s key lies in its ability to differentiate soft tissues – it can even tell the difference between infected and normal tissues. Infections within bones are best identified using MRI, and then surgeons can plan whether to treat with antibiotics, an operation, or if the infection is spread too far, an amputation.
MRI Scanner Construction and Work
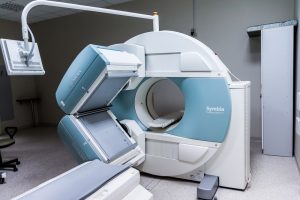 It’s a big, hi-tech machine and there are different varieties all around the world, found in hospitals, medical research centres and even zoos, but they all work on common principles of manipulating the laws of physics.
It’s a big, hi-tech machine and there are different varieties all around the world, found in hospitals, medical research centres and even zoos, but they all work on common principles of manipulating the laws of physics.
Radiofrequency transmission – A radiofrequency transmission causes the protons to flip around, and then turning this off causes the protons to re-align. This movement releases energy that is detected by the scanner to create pictures.
Enhancement – Contrast agents are used in addition to enhance the contrast between tissue types. For looking at joints such as the shoulder or knee, contrast can be injected directly into the joint prior to the scan. For the blood vessels, an intravenous contrast is injected during the scan.
Bang bang! – The gradient coils are switched on an< off rapidly and alter the magnetic field in specific tissue areas. As they switch on and off, the coils contract and expand by tiny amounts. This produces a loud noise which is heard as a series of loud bangs.
Looking for tumours – Since the protons in different tissue types return to their normal state at different rates, they give off different frequencies of energy and so contrast between different types of tissues can be seen. This allows identification of a brain tumour from normal cells.
Gradient coils – These coils produce much weaker, variable magnetic fields compared to the superconductors. These gradient fields are specifically targeted to certain tissues, allowing for depth and detailed tissue type differentiation.
Superconducting magnets – These powerful magnets create very stable magnetic fields, which align protons within the body’s hydrogen atoms. The magnets are cooled to near absolute zero and so are well insulated from the patient.
The tunnel – The tunnel which the patient lies in is very narrow; some patients don’t fit. There are small lights and a radio with headphones to keep you comfortable.
The computer – Once the changes in energy have been detected within the scanner, they are transmitted to powerful computers outside the scanner, which transform the data into useful images.
Lie table – The patient lies down on a narrow plastic ‘table’ outside the machine, which is then advanced slowly into the tunnel.
According to the intensity of the magnetic field MRI scanners are divided into:
- low field strength devices – up to 0.5 T
- medium field strength devices – 0.5 T to 1 T
- high field strength devices – 1 T and above (1.5 T, 2 T, 3 T, 7 T, …)
MRI Scanner facts
 Careful – Due to the powerful magnets, any metal objects left in the room can be pulled towards the magnet and can harm patients. Examples have included oxygen cylinders and chairs.
Careful – Due to the powerful magnets, any metal objects left in the room can be pulled towards the magnet and can harm patients. Examples have included oxygen cylinders and chairs.
Pacemakers – Pacemakers were absolute contraindications to MRI scans; modem pacemakers and implantable defibrillators, however, are being designed to be ‘MRI safe.’
The most modern – MRI scans can be combined with PET scans. These PET-MRI scans produce anatomical and functional images, such as assessing for extent of tumour growth and tumour activity.
Now that’s cold – The coils of the superconducting magnets are cooled to lower their resistance. Liquid helium cools them to near absolute zero (around -270”C).
Mobile MRI – Mobile MRI scanners can go to the patients. They are based in big articulated lorries and can be stationed outside hospitals to provide extra scanning capacity.